The silent pandemic
Bacteria often colonize the human body without causing disease — but they can also lead to serious infections. Scientists at the Helmholtz Institute Würzburg are looking for new targets in various germs, as conventional antibiotics are becoming increasingly ineffective.
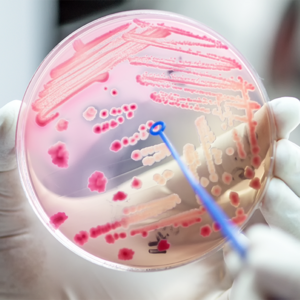
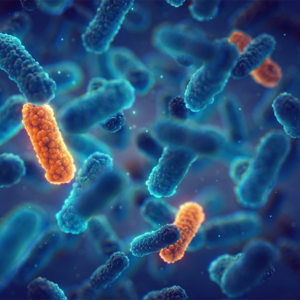
They are known as "Klebsiella", "Escherichia coli" and "Staphylococcus ", they are found on the skin and mucous membranes, in the intestines or, for example, in the lungs, and they share a common feature: such bacteria often colonize the human body without causing any disease — but they can also lead to serious infections.
Immunocompromised patients can be particularly affected, making Klebsiella & Co. spread fear as so-called hospital germs. And even worse: due to overuse and misuse of conventional antibiotics, the pathogens have now developed a variety of defense strategies that make standard active agents increasingly ineffective.
The World Health Organization (WHO) estimates that more than one million people worldwide die every year as a result of infections caused by multi-resistant pathogens. By 2050, figures could rise to ten million deaths — unless new antimicrobial drugs can be developed.
A promising approach
To fight antibiotic resistance, to develop targeted therapeutics and to contain tumor-promoting bacteria, scientists at the Helmholtz Institute for RNA-based Infection Research (HIRI) and Julius-Maximilians-Universität (JMU) in Würzburg are looking for new targets in various germs.
Programmable antibiotics, so-called antisense oligonucleotides (ASOs), are a promising new approach. They are being researched in the laboratory of HIRI Director Jörg Vogel. ASOs target the messenger ribonucleic acids (mRNAs) which bacteria require to synthesize new proteins and replicate. As a mirror-image structure of a bacterial mRNA, specifically programmed ASOs can bind to it and deactivate it.
“We introduce short chains of bases into bacteria that are designed to exactly match specific genes,” explains Vogel. “When these chains bind to the corresponding mRNA of the gene of interest, they abrogate protein production and, ideally, the bacterium dies as a result.”
However, according to the professor, it is a challenge to get the relatively large antisense RNA molecules through the complex bacterial cell wall into the cytoplasm. "In my laboratory, we are investigating how small the snippets can be kept without them losing their specificity," reports Jörg Vogel. Specificity means that only the gene of interest will be blocked and non-specific binding to mRNA of other genes will be avoided.
In addition, the programmed antisense RNA is bound to a peptide or carbohydrate ligand, Vogel says. Receptors on the bacterial cell wall recognize this molecule complex and let it enter the cell. The first drugs that work via this principle are already on the market, such as those for treatment of the consequences of spinal muscular atrophy or hepatitis C infection.
However, mRNA antibiotics have been confined to the laboratory so far, though there would be a wide range of potential applications. Various microorganisms could be precisely targeted or even completely destroyed, from hospital germs to fusobacteria, which are associated with intestinal and breast cancer, to sweat-decomposing microbes. And all without causing undesirable dysbiosis, i.e. without damaging the "good" bacteria of the microbiota, as is the case with conventional antibiotics.
The low turnover that the pharmaceutical industry can generate with a newly developed antibiotic — coupled with high costs at the same time — is the stumbling block in research and drug development to date.
Background
A piece on the occasion of the "World Antimicrobial Resistance Awareness Week" (WAAW; November 18 – 24, 2023): Every year in November, the World Health Organization (WHO) together with the Food and Agriculture Organization of the United Nations (FAO), the United Nations Environment Programme (UNEP), and the World Organisation for Animal Health (WOAH) use WAAW to draw attention to the importance of antimicrobial agents and the problem of resistances. This year's motto is "Preventing antimicrobial resistance together".

Official campaign asset of the #WAAW. © FAO / UNEP / WHO / WOAH
Helmholtz Institute for RNA-based Infection Research
The Helmholtz Institute for RNA-based Infection Research (HIRI) is the first institution of its kind worldwide to combine ribonucleic acid (RNA) research with infection biology. Based on novel findings from its strong basic research program, the institute’s long-term goal is to develop innovative therapeutic approaches to better diagnose and treat human infections.
HIRI is a site of the Braunschweig Helmholtz Centre for Infection Research (HZI) in cooperation with the Julius-Maximilians-Universität Würzburg (JMU) and is located on the Würzburg Medical Campus.